top of page
Osteitis pubis/adductor tendonitis

What is osteitis pubis?
What is osteitis pubis?
Osteitis pubis is an umbrella term that describes a few conditions all causing pain around the pubic symphysis. The pubic symphysis is a small joint at the front of the pelvis in the body's midline, immediately above the genitals. The two bones on each side of the joint (called the pubic bones) provide attachments to the muscles of the inner thigh and the abdomen and, therefore, can undergo stress due to sports or repeated activities. Osteitis pubis is more common in men, particularly if doing sports and in pregnant ladies.
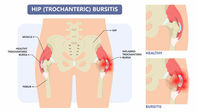
Relevant anatomy
The pubic symphysis is a small joint at the front of the pelvis. It is formed by the two pubic bones meeting together in the midline. The joint has a fibrous disc in the centre and the bones are connected together by strong ligaments. In addition, the pubic bones attach to the adductor muscles (the muscles at the inner aspect of the thigh) and the rectus abdominous (the six-pack) muscles. Therefore, the joint undergoes a lot of force during sports activities like running and football.


What are the causes of osteitis pubis?
Osteitis pubis is a repetitive stress-type injury. It is more common in men and often seen in sports people. The pubic symphysis and the adjacent structures undergo repeated forces secondary to overuse. This will overload the pubic symphysis and the adjacent stabilising structures, resulting in injury.
Osteitis pubis includes a few conditions and can be referred to by a few names, resulting in pain in the groin region.
-
It is sometimes called "athletic pubalgia", meaning groin pain in people who do athletic activities.
-
"Osteitis pubis"- Refers to increased stress upon the pubic bone, which provides attachments to essential tendons and ligaments in this area, or if there is instability of the pubic symphysis.
-
"Adductor tendonitis" refers to Inflammation/irritation of the adductor tendons that attach to the pubic bone. In more advanced cases, there could be a tear to the adductor tendon attachment. An ultrasound will be very useful in establishing the diagnosis and assessing the integrity of the tendons.
-
Sometimes, the condition is referred to as a “sports hernia”. Although there is no actual hernia here, the nomenclature reflects that the condition is more common in sports people and results in groin pain (the same site of pain when there is a true hernia).
-
Osteitis pubis can also happen during pregnancy or childbirth, but the discussion of this is beyond the scope of this article.
The underlying cause for the pain can be complex, given the complex anatomy of the structures that could be involved here. Therefore, imaging assessment plays a vital role in establishing the correct diagnosis. A hip MRI examination would be very useful for the assessment.


What are the clinical features of osteitis pubis?
The main symptoms of osteitis pubis are:
-
Pain over the pubic symphysis/groin region. The pain usually starts gradually as a mild discomfort, particularly after activities. It can progress causing significant discomfort and interfering with simple things like walking.
-
The pain can be referred to the inner aspect of the thigh or the lower abdomen, at the site of the tendons' attachment to the bone.
-
The pain can be more severe after sports that involve sudden changes in speed and direction (like football).
What conditions can mimic osteitis pubis?
Osteitis pubis can be mistaken for a number of other hip problems. These include:
-
Inguinal hernia. This is usually associated with a feeling of pressure and focal groin swelling, particularly on straining. Ultrasound is an excellent modality for the assessment of suspected groin hernia, as it allows for dynamic assessment. To find out more, please read our article about groin hernia.
-
Stress fracture. If the stress changes within the pubic bone progress, they can lead to a stress fracture.
How is osteitis pubis diagnosed?
Detailed clinical assessment by a specialist orthopaedic doctor is essential. Imaging is almost always required to confirm the diagnosis and assess the severity of the condition. Ultrasound can be useful for the assessment, but given the complexity of the anatomical structures here, an MRI hip examination would provide a more detailed assessment. In addition, ultrasound can not assess the bony changes of osteitis pubis, while MRI would readily demonstrate these. MRI is also very sensitive in assessing the presence of any tear to the adductor or rectus abdominous muscles. Ultrasound guidance is extremely useful when injecting the area. There is plenty of evidence showing that injections done under ultrasound guidance result in better outcomes, with better pain relief and improved function. A hip X-ray will provide useful information about the pubic symphysis and assess the joint alignment but will not assess the soft tissues, ligaments, and tendons. Sometimes, a pelvis stress x-ray is performed by obtaining a film while the patient is standing on one leg to check for any pubic symphysis instability.

A hip xray showing normal alignement of the pubic symphsis
What is the treatment for osteitis pubis?
Management usually starts using conservative measures like physiotherapy, patient education and exercise modification. Physiotherapy will usually consist of a progressive rehabilitation program to stretch and strengthen the hip muscles. It is important to avoid asymmetrical posture when standing as this will put extra stress on the affected side. Some patients find it helpful by placing a pillow between their legs when going to bed. Oral anti-inflammatory tablets can be also useful in the management.
What are the different injection treatment options for osteitis pubis?
If the above conservative measures do not result in a satisfactory response, then an ultrasound-guided injection can be considered. The options include:
-
Injecting a small dose of steroids close to the adductor tendons reduces inflammation and helps with the rehab program. To find out more, please see our article about ultrasound-guided hip steroid injections.
-
Other options include platelet-rich plasma (PRP) injections and tenotomy. In PRP injection, a blood sample is taken from your vein and put in a special centrifuge machine to separate its different components. The layer on the top is called “the plasma” which contains the platelets and other useful growth factors. This is injected into the tendon under ultrasound guidance to help stimulate healing. Please see our PRP injections article for more details. In tendon fenestration/tenotomy, a small needle is used to fenestrate the inflamed tendon multiple times under ultrasound guidance. This is thought to result in the release of certain factors that help in tendon healing. If the cause of the pain is more related to the pubic symphysis, then an ultrasound-guided steroid injection into the pubic symphysis joint can be considered.
Should adductor tendon injections be done under ultrasound guidance?
Yes. This is our routine practice as there is plenty of evidence supporting the use of ultrasound guidance when performing musculoskeletal injections. Doing injections under ultrasound/imaging guidance allows for direct visualization of the needle to ensure accurate placement into the area of pain/inflammation (like a bursa, an arthritic joint, or an inflamed tendon sheath). Ultrasound guidance results in more accurate, less painful, and faster procedures, with better outcomes, compared to doing these injections without guidance. Ultrasound guidance ensures the avoidance of any sensitive structures (like nerves and vessels) during the procedure.
What are the possible side effects of a steroid injection?
Generally, these injections are very safe and routinely done in our practice. There is a very small risk of infection (about 1:10.000). The injected area may feel sore for the first few days. This is referred to as (steroid flare) and can be seen after a steroid injection. The procedure will be explained to you in detail during your appointment and all your questions will be addressed. To find out more about cortisone injection in general, please see our FAQs.
How long will the effect of a hip cortisone injection last?
Current evidence suggests that cortisone can improve pain and function for up to 3 months, but in some cases, it can last longer. The injections usually also contain a local anaesthetic that provides immediate pain relief lasting a few hours.
How soon will a steroid injection start to work?
A steroid injection usually takes a few days (1-3) before you notice the effect, although sometimes the pain relief can start on the same day. More commonly, the injected area will feel sore for the first few days. This is referred to as (steroid flare) and can be seen after a steroid injection.
How many steroid injections can I have for osteitis pubis?
We advise reducing the number of cortisone injections if possible, by combining any injection therapy with an effective physiotherapy program to address the underlying cause. Repeated steroid injection into the same area should be avoided if the previous injection was less than 3-4 months ago.
How long should I rest after a hip injection?
Usually, we advise patients to rest for 48-72 hours after having a hip injection. This can vary depending on the type of treatment and severity of the condition. Usually, patients who have a steroid injection are usually advised to rest for 48 hours, while patients who had a more advanced procedure like PRP injection into the tendons may be advised to rest for 5-7 days.
Recent posts
Related posts
Other conditions
Categories
Causes of osteitis pubis
Clinical features
Conditions that can mimic osteitis pubis
Diagnosis
Treatment
Ultrasound-guided injections
FAQs about osteitis pubis
Hip conditions and treatments
-
Adductor tendinosis/tear

Specialist Consultant Musculoskeletal Radiologist Doctor with extensive experience in image-guided intervention
To book a consultation
Call us on 020 8050 9885 or Book online
The Musculoskeletal Ultrasound & Injections clinic
Brentford, TW8 9DR

bottom of page