What is knee aspiration?
- Dr. Zeid Al-Ani

- Feb 7, 2023
- 4 min read
Updated: Apr 12, 2023
When there is excess fluid within the knee, this is referred to as joint effusion. It can result in knee swelling, pain and restriction of movement. Treatment of mild cases consists of rest, ice packs and anti-inflammatory tablets. In resistant cases or if the joint effusion is sizeable, then ultrasound-guided aspiration can be useful for the management. Knee aspiration refers to draining this excess fluid from the knee joint.

What are the causes of fluid build-up within the knee?
The knee joint is lined by a special type of tissue (called synovium) and it is responsible for the production of a special type of fluid within our joints (called the synovial fluid). This plays an important role in joint function and lubrication, ensuring smooth and frictionless movement and protecting the cartilage. However, if the knee joint is irritated which could happen secondary to an injury (like a meniscal tear) or due to a degenerative process (like knee osteoarthritis), then joint will produce excess fluid within the joint. Other causes for excess fluid within the joint include infection and inflammatory type arthritis (like rheumatoid arthritis).
What is the best knee scan to assess for fluid within the knee?
X-ray would be very useful to assess for knee arthritis changes. Ultrasound is useful in assessing for presence of fluid within the knee and its size. It is also useful to perform ultrasound-guided aspiration. MRI is useful to assess the internal structures of the knee (like a meniscal tear) trying to establish the reason for knee effusion.
When to consider knee aspiration/drainage?
The two main reasons to consider knee joint aspiration (drainage) are:
1. If further assessment of the fluid would be useful to know what is happening. I.e. if the obtained fluid would help tell us the diagnosis. There are certain types of arthritis (like gout) where examining the joint fluid can confirm the diagnosis. Fluid aspiration is also usually done when we suspect there is knee joint infection (called septic arthritis) as the obtained fluid will confirm the diagnosis and also help in deciding the most suitable antibiotic treatment option, depending on the type of the bacteria causing the infection.
2. If there is large volume of fluid within the knee that is causing pain and limitation of joint movement. Removal of fluid usually results in relief of the symptoms. Sometimes, the aspiration procedure is combined with a knee joint cortisone injection to help settle down the inflammation.
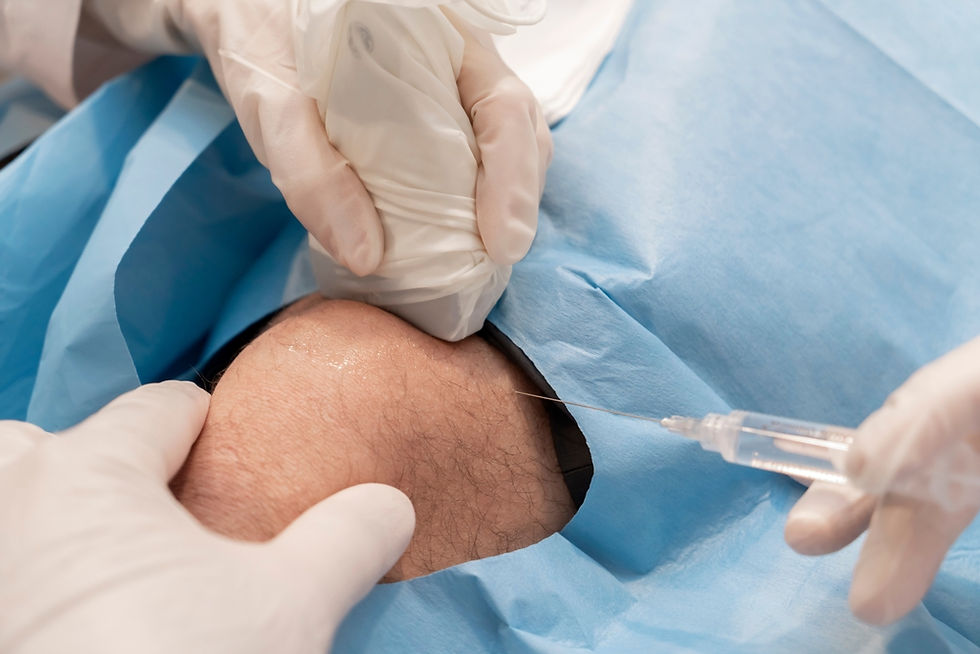
How knee joint aspiration procedure is done?
First the doctor will use ultrasound to scan the knee and find the best place to perform the procedure. The procedure is done in a clean clinic room using aseptic (extremely clean) technique. The skin will be cleaned using an antiseptic solution. All the equipment used will be sterile (sterile pack, sterile gloves and sterile probe cover). Usually a small amount of numbing medicine (local anaesthetic) will be used initially. A needle will then be inserted into the fluid (usually above the knee cap) under ultrasound guidance and the fluid will be aspirated. If the fluid within the knee is due to inflammatory or degenerative cause, an ultrasound-guided knee joint steroid injection may be performed at the same time. Other injection therapies like intra-articular Hyaluroinc acid and PRP injections can be also performed at the same time. Then a small plaster will be applied to the skin. Using ice packs and anti-inflammatory tablets usually help in the management and prevent (or reduce the possibility of) the fluid from coming back.
What are the risks from a knee aspiration?
Generally, a knee joint aspiration is very safe and routinely performed. There is very small risk of introducing infection (about 1:10000) but this is minimised by using clean technique as described. If the area of aspiration or the knee become hot, red, painful and swollen after the procedure and the symptoms are not settling, then this could be due to infection. You should see a Doctor urgently if such symptoms develop.
Sometimes, the fluid within the knee is thick and therefore difficult to drain.
There might be a possibility of fluid recurrence after the drainage procedure (depending on the cause of fluid build-up and any on-going treatment). Therefore, it is important to address any underlying cause for fluid accumulation within the knee joint (for example treating a meniscal tear or gout). Combining the aspiration with a steroid injection (in conditions such as knee joint osteoarthritis) will be useful to reduce the chance of recurrence.
What is the benefit of doing knee aspiration under ultrasound-guidance?
Ultrasound increases the accuracy of the procedure as it will direct the needle to the exact site of fluid. Also, it is safer as the adjacent important structures can be visualised and avoided using ultrasound. Patients usually report less pain during the procedure when it is done with ultrasound-guidance.

What to do after knee joint aspiration?
A small plaster will be applied to the skin. The doctor will inform you when you can remove this. The needle entry site should stay clean to prevent infection. Usually rest is advised for the first 48 hours after the procedure. The procedure usually involves injecting a small amount of numbing medicine, therefore, you will be advised not drive for a few hours, until the effect of the numbing medications wear off.
Can knee joint effusion seen with a Baker’s cyst?
Yes, Baker’s cyst refers to focal accumulation of fluid at the back of the knee and can be associated with excess fluid within the knee (effusion). To find out more, please read our article about Baker’s cyst.
Knee conditions and treatment